 |
Four Hidden Lifestyle Risks Associated with Dry Eye
How ODs can help their patients reduce the expression of DED in their daily lives.
By Tracy Doll, OD
Release Date: May 15, 2022
Expiration Date: May 15, 2025
Estimated Time to Complete Activity: 2 hours
Jointly provided by Postgraduate Institute for Medicine (PIM) and Review Education Group
Educational Objectives: After completing this activity, the participant should be better able to:
- Recognize the different factors that contribute to dry eye disease.
- Explain how a patient's lifestyle can exacerbate the condition.
- Educate patients on changes that can help reduce the expression of DED.
- Communicate effectively to patients about dry eye disease.
Target Audience: This activity is intended for optometrists engaged in managing dry eye.
Accreditation Statement: In support of improving patient care, this activity has been planned and implemented by PIM and the Review Education Group. PIM is jointly accredited by the Accreditation Council for Continuing Medical Education, the Accreditation Council for Pharmacy Education and the American Nurses Credentialing Center to provide CE for the healthcare team. PIM is accredited by COPE to provide CE to optometrists.
Reviewed by: Salus University, Elkins Park, PA
Faculty/Editorial Board: Tracy Doll, OD
Credit Statement: This course is COPE approved for 2 hours of CE credit. Activity #123894 and course ID 78368-TD. Check with your local state licensing board to see if this counts toward your CE requirement for relicensure.
Disclosure Statements: PIM requires faculty, planners and others in control of educational content to disclose all their financial relationships with ineligible companies. All identified conflicts of interest are thoroughly vetted and mitigated according to PIM policy. PIM is committed to providing its learners with high-quality, accredited CE activities and related materials that promote improvements or quality in healthcare and not a specific proprietary business interest of an ineligible company.
Those involved reported the following relevant financial relationships with ineligible entities related to the educational content of this CE activity: Author: Dr. Doll receives fees from Dompé, Oyster Point, Science-Based Health, Kala, Cynosure and Sun Pharma. Managers and Editorial Staff: The PIM planners and managers have nothing to disclose. The Review Education Group planners, managers and editorial staff have nothing to disclose.
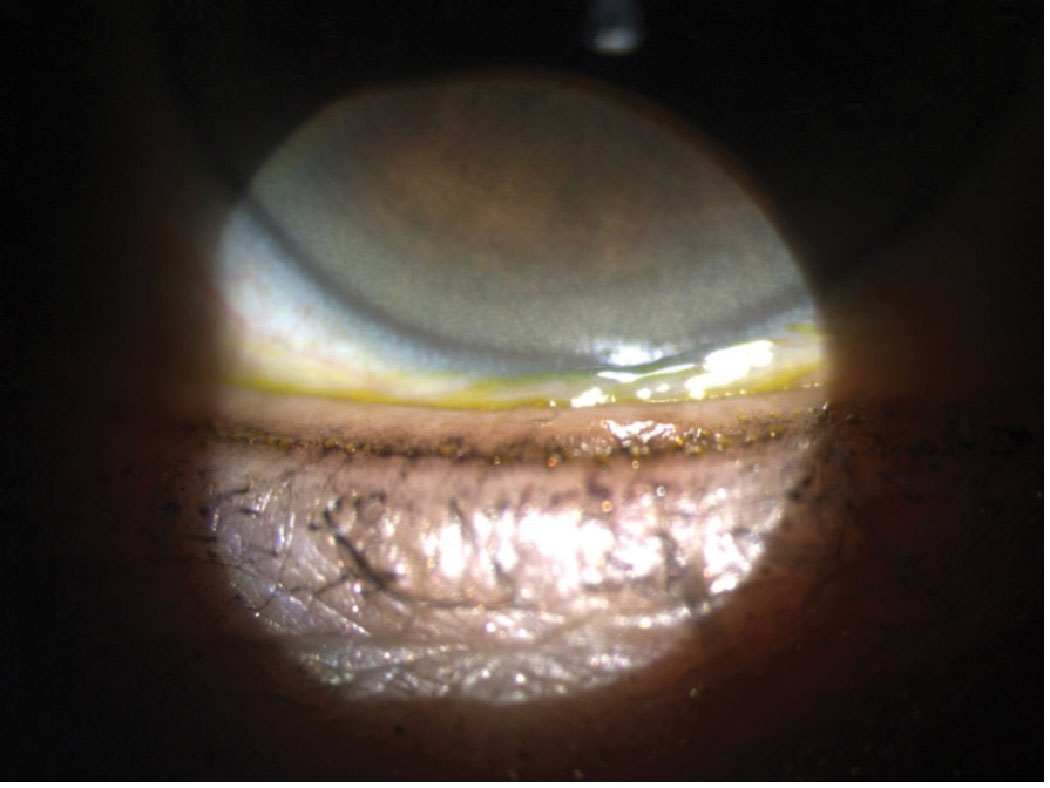 |
| Fig. 1. Tight-lining/water-lining with eyeliner. Click image to enlarge. |
Dry eye is one of the most common ocular issues an optometrist will encounter in their practice. The classic risk factors for ocular surface dryness have been well discussed and documented for over a decade, thanks in part to the oft-quoted body of evidence-based papers reported by the Tear Film and Ocular Surface Society (TFOS) DEWS I and DEWS II reports.1,2 Older age, female sex, history of ocular surgery, contact lens wear and comorbid systemic disease are well-known culprits of ocular surface dryness. The classic dry eye patient is still women over the age of 50.
While some risk factors cannot be changed, newer investigations are seeking ways to prevent ocular surface dryness from being compounded by preventable lifestyle risk factors. TFOS is currently investigating these modifiable risks, which will be discussed in the group’s upcoming workshop, “A Lifestyle Epidemic: Ocular Surface Disease.”3
The picture of ocular surface dryness is changing and becoming more inclusive of broader patient types, including younger individuals. This article seeks to highlight four lifestyle risk factors that may be present for both classic and non-classic patients alike. The vicious cycle of chronic ocular surface dryness can be initiated by regular ocular surface irritation. The daily lifestyle habits described in this article all lend themselves to habitual ocular irritation.
Risk Factor #1: Cosmetics
The most common eye cosmetics in the marketplace continue to be mascara and eyeliner, followed by eyebrow makeup and eyeshadow.4 And thanks to the Zoom effect, we are aware of our appearances now more than ever before.5 Never before have individuals had to work and socialize with a virtual mirror in place. Multiple surveys have indicated increased interest in improving the physical appearance of the eyes through both cosmetics (skincare/makeup), cosmetic enhancements and surgical means.5-8
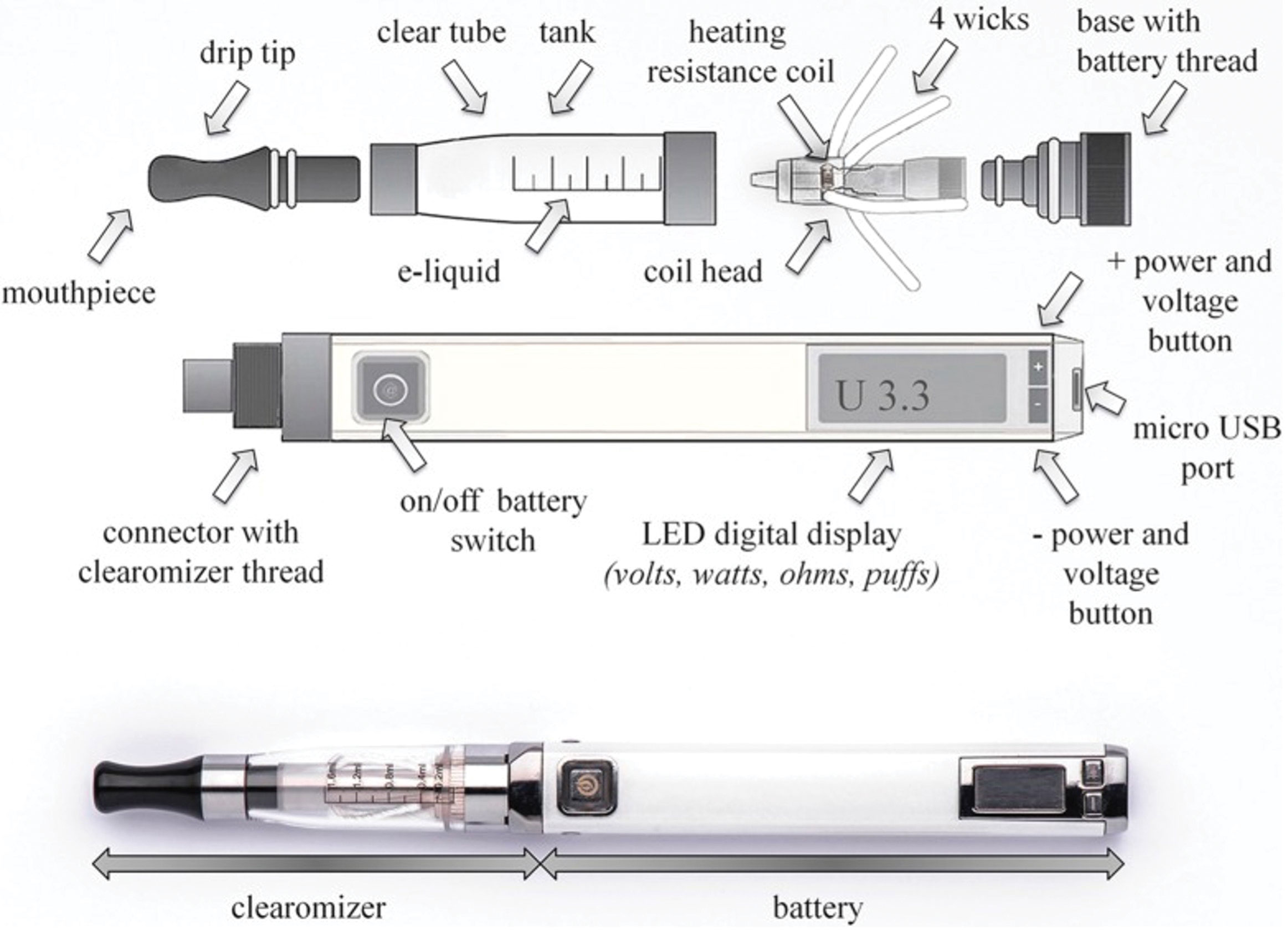 |
| Fig. 2. The basic construction of a vaping mod.75 Click image to enlarge. |
Sadly, consumers have been led to trust marketing terms that have no specific regulation or definition in the United States cosmetics and makeup marketplace. The following terms are not currently standardized in the United States: hypoallergic, clinically tested, doctor recommended, natural and pH balanced.8-16 With no standards, health benefits cannot be verified. In fact, only 11 ingredients have been banned from cosmetics in this country compared with the nearly 1,300 substances banned in the European Union.9 The burden currently lies with the consumer to read the ingredients listed on product packaging to determine cosmetic safety.
With multiple scientific and lay terms for individual cosmetic ingredients, this task can be particularly daunting. The eyecare provider can be helpful in educating patients about the most common eye cosmetic irritants and offering credible resources. It should be noted that interactions between individual ingredients and the impact of layering cosmetics have not been well documented or investigated. This is an area that needs further study.
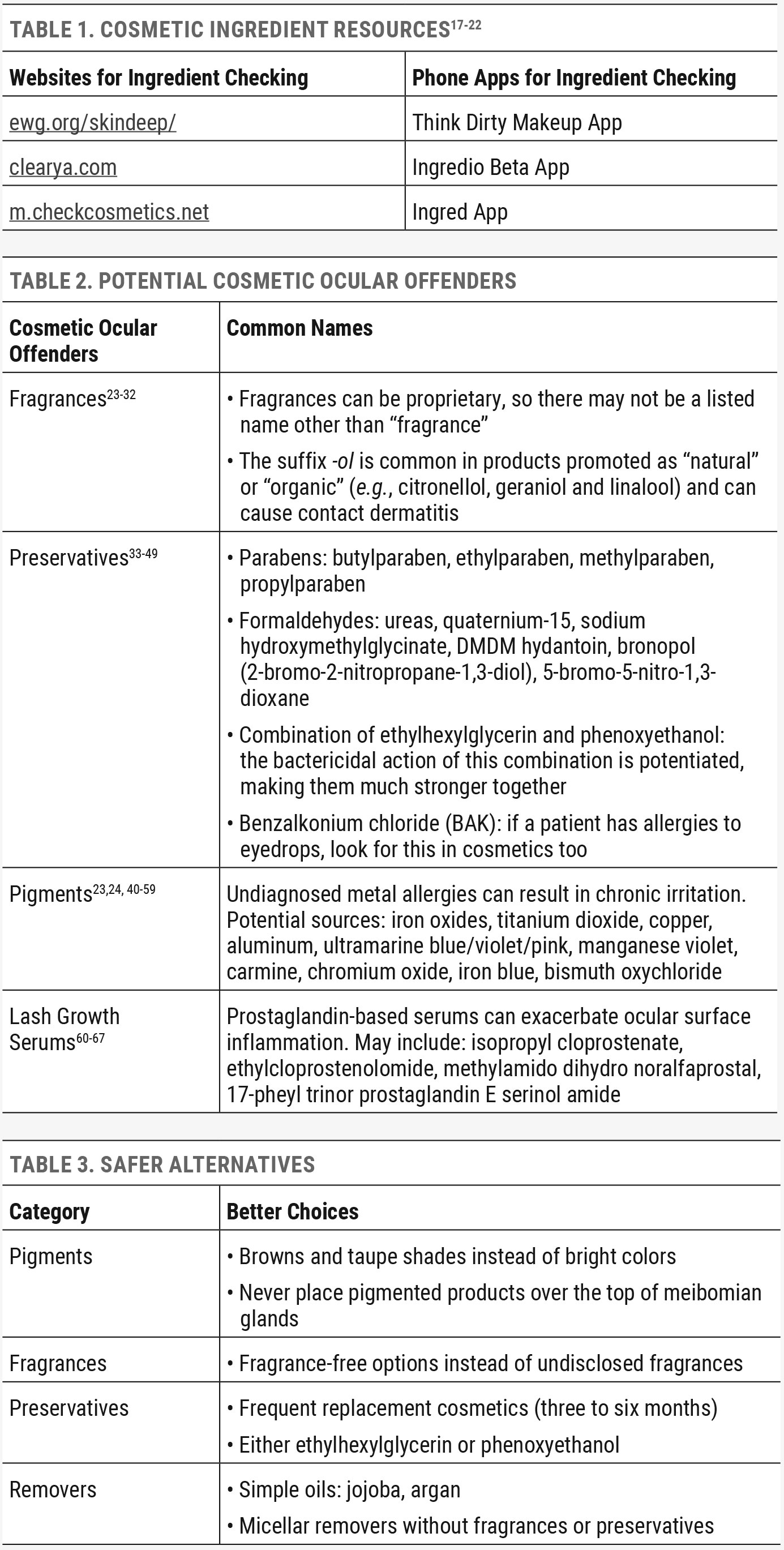
There are a number of cosmetic ingredients that can be considered ocular surface offenders, and it is important that patients be made aware of the associated risks. Before purchasing an eye cosmetic, recheck the packaging for known allergies and irritants. Manufacturers can change ingredients in cosmetics without warning. Fragrance as an ingredient can be particularly tricky, as they are considered proprietary and their exact composition is not required to be listed.23-32 A healthier option for ocular cosmetics can be to choose fragrance-free products. Preservatives are helpful to prevent bacterial growth in cosmetics but can also kill off the natural and healthy flora responsible for maintaining proper lipid barrier function of the skin on the eyelids.33-49 Choosing cosmetics with more frequent replacement and lower levels of preservatives is a better balance vs. cosmetics with multiple harsh preservatives.
 |
| Click to enlarge. |
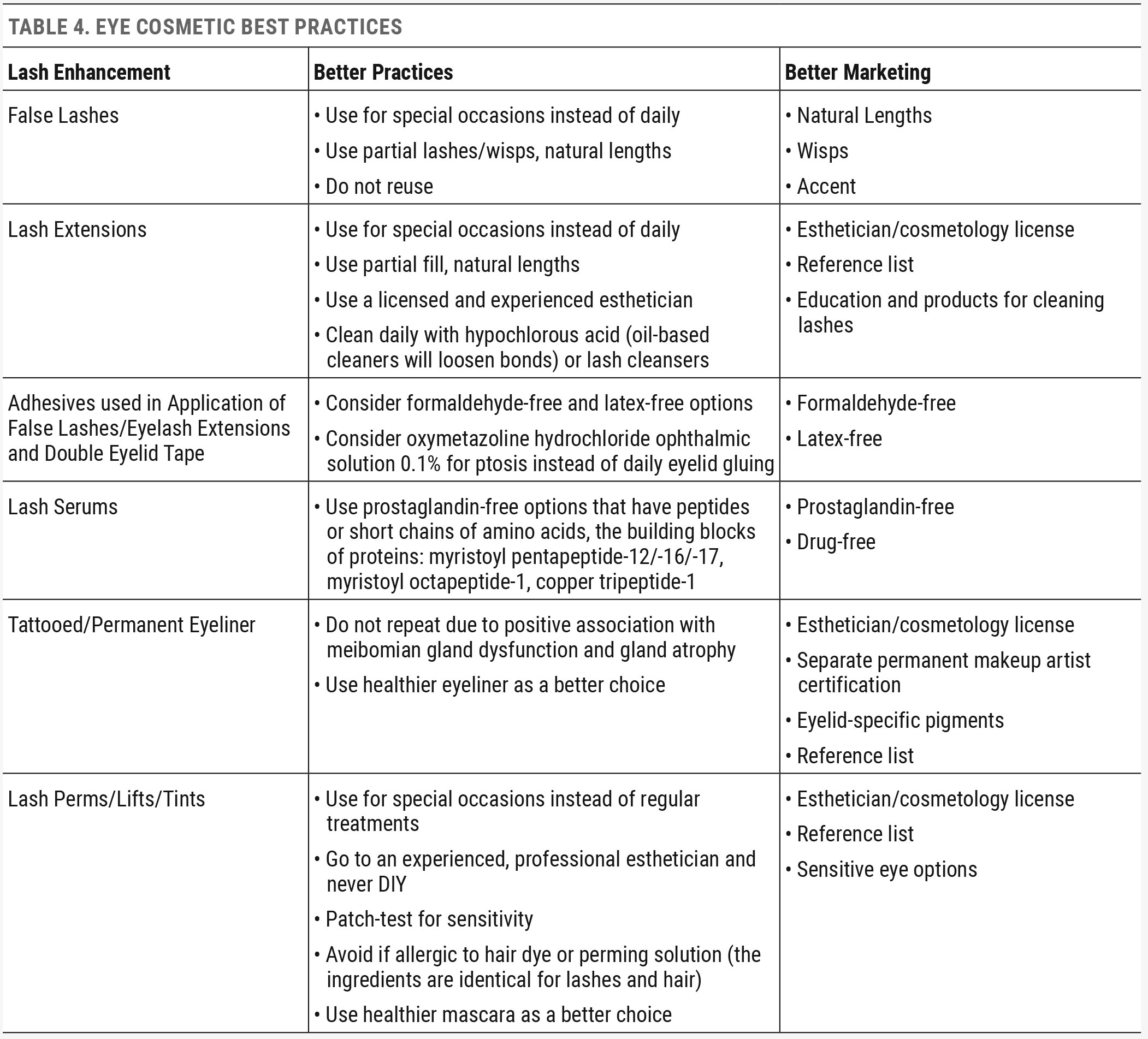
Other, less eye-irritating cosmetic swap-outs can be encouraged. One example would be to choose a one-ingredient oil (argan or jojoba oil) as an eye makeup remover instead of a 14-ingredient oil-free option packed with multiple preservatives, dyes and fragrances. Colorful cosmetics should also be used in moderation. A general rule to follow: the more colorful, the higher the potential for causing eye irritation. It’s better to stick with neutral tones of brown and taupe vs. blues, pinks and purples.23,24,40-59 It’s also a much healthier idea to avoid placing pigmented products over the top of the meibomian glands, as they can contain waxes and irritating pigments. Tight-lining or water-lining with eyeliner should be moved a few centimeters away from the gland openings.
The addition of ocular cosmetic enhancements has compounded the potential for ocular surface irritation. The growing trend of false eyelashes is dominating the eye beauty market. Eyelashes are not simply beauty adornments but rather serve the very specific anatomical function of diverting debris from the ocular surface. The ideal eyelash length determined to be helpful in mammals (animals and humans alike) is one-third the eye width.68 Altering this ratio could result in a wind tunnel effect, funneling allergens, dust and debris right to the ocular surface.68 Before healthcare providers consider capitalizing on this trend, careful thought should be given to anatomical function. When considering options for safer cosmetic lash and lid enhancement, the healthiest choices are temporary, removable and applied by experienced and licensed aestheticians. Generally, beauty enhancements requiring licensure should not be DIY.
Most people do not discard cosmetics appropriately, and cosmetics can become contaminated with skin flora. Thirty percent of single-user mascaras are contaminated with overgrowth of bacteria at the three-month mark.69 For this reason, all liquid cosmetics should be replaced at least every three months. Powders are also not immune to bacterial growth and should be replaced every four to six months.
Additionally, cleaning applicators is very important to avoid overgrowth of micro-organisms and invasion from non-native species, including fungus.70-73 Infected cosmetic tools present a risk for soft tissue infections if the epidermis is not intact. Makeup sponges harbor the most bacteria due to their large surface area and ability to hold moisture. Weekly cleaning of cosmetic applicator tools (e.g., brushes, sponges) with most types of soaps or alcohol-based cleansers has been shown to be adequate in reducing microbial levels of Staphylococcus and Streptococcus species on cosmetic applicators.74 All cleaned brushes ideally should be stored in cool, dry locations.
Risk Factor #2: Vaping
The origination of the e-cigarette/vaping module came from a good place: the desire to deliver nicotine without the harmful effects from the carcinogenic ingredients in classic tobacco cigarettes. The original devices were even made to look like classic cigarettes. However, they have evolved over time to look less like a cigarette and to be more discreet; some even look like pens, AirPod cases or USB flash drives. Regardless of technology, all vaping mods have a basic construction: a metallic coil is immersed in vaping fluid containing the substance of choice, most commonly nicotine (cannabinoids are also common).75-77 A battery sends an electric current through the coil, resulting in heating and vaporization of the juice, which is then inhaled. The strength of the e-cigarette/vape battery (lithium-ion) output is what determines the amount of nicotine and vapor that is produced with every inhale and exhale.
 |
| Fig. 3. Be mindful of harmful substances on a cosmetic product’s ingredient list. Click image to enlarge. |
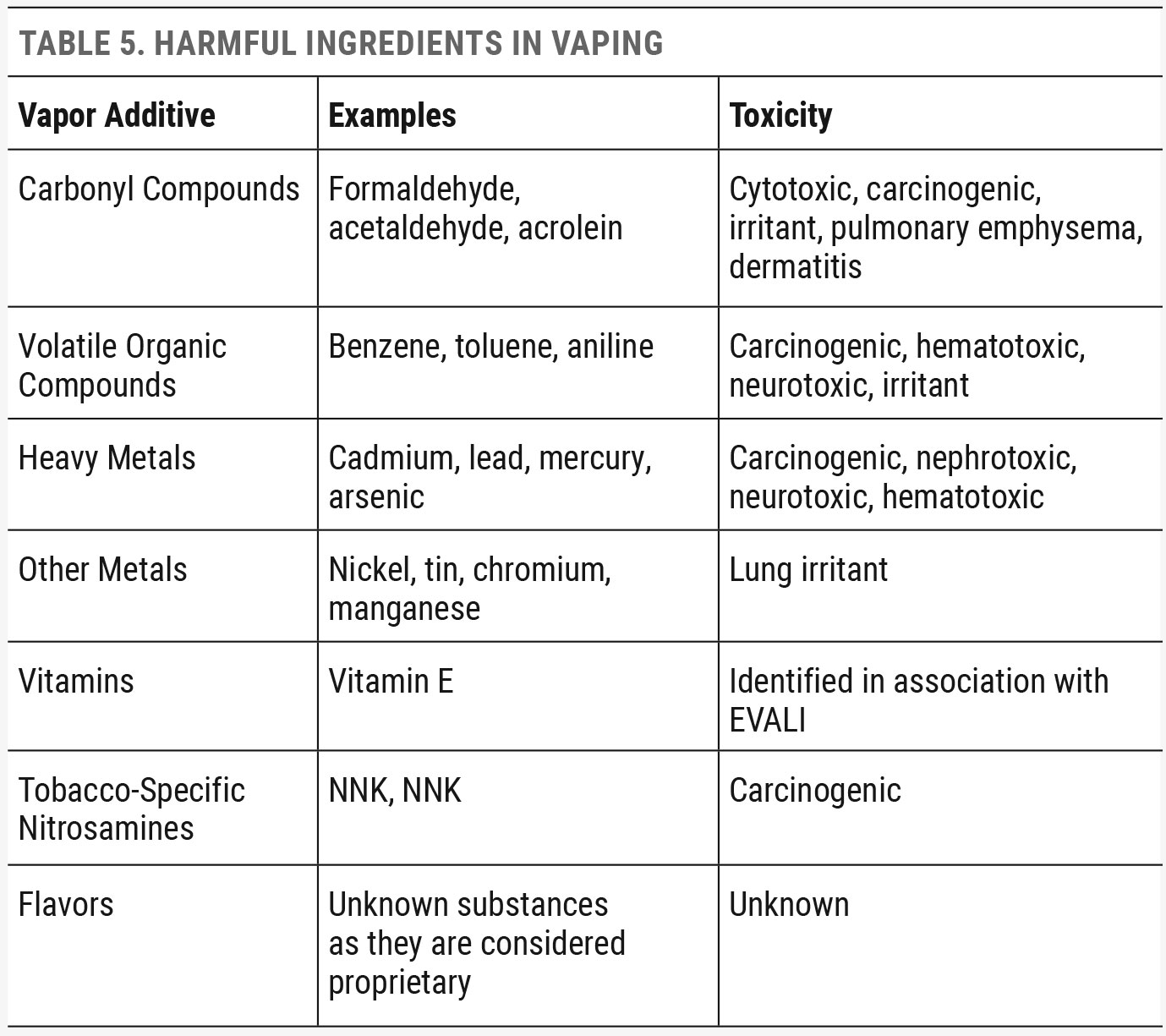
Sadly, while these devices are arguably less harmful than tobacco cigarettes, they are not without health risks. Like cosmetics, there is poor regulation of the over 80 known ingredients in vaping juice. The most common juices have nicotine solubilized in propylene glycol or glycerin. Nicotine alone in water vapor feels very harsh, resulting in a peppery sensation on the back of the throat. Unfortunately, vaping juice solvents have been associated with a lung condition mimicking pneumonia, known as EVALI (e-cigarette or vaping-associated lung injury).78-80 The heated metallic coils can also leach metals into the vaping juice, resulting in metal deposition in the lungs.
These known toxic and carcinogenic ingredients, when exhaled, can also make their way to the ocular surface. Vaping has been positively associated with disrupting the lipid layer of the tear film, causing ocular surface dryness.81-87 Reduction in noninvasive corneal tear breakup time and tear breakup time has been associated with vaping. Higher voltage with more chemical release has been correlated with worsening symptoms, Shirmer score and tear stability.81-87
In addition to the impact on the tear film, there lies the potential for severe vision loss with improper modification of vaping mods. Batteries that are improperly combined with combustion units to create higher levels of delivered nicotine (or other substances) could result in device explosion. There are documented cases of explosive foreign bodies, including metallic shrapnel imbedding in the ocular tissues.88-90 Patients need to be reminded of this risk and to never combine non-approved device components.
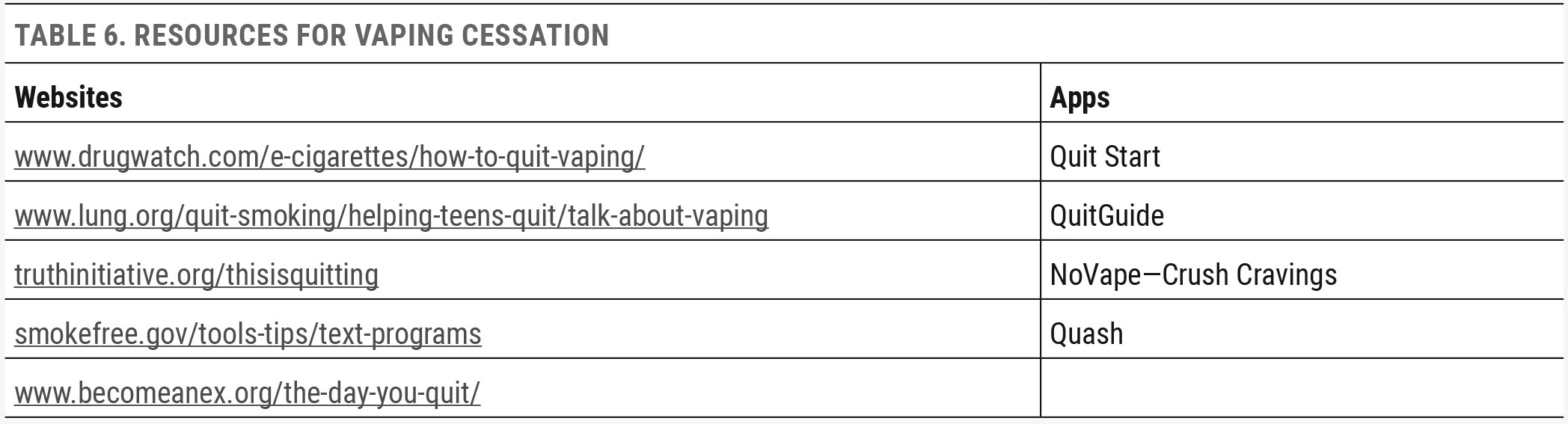
The eyecare provider should be very specific when taking case history. It is important to ask about vaping in addition to smoking because patients may not identify vaping and smoking as the same act. In the early days of vaping modules, the marketing was very clearly aimed at a younger population, using candy flavors, bright colors and young models in marketing. Since the appearance of vaping devices in the mid-2010s, many states have adopted laws mandating that vaping device and juice companies eliminate colorful packaging and flavoring that would appeal to minors. Unfortunately, these laws may have come too late. A survey in 2021 indicated that 11.3% of high school students (1.72 million) and 2.8% of middle school students (320,000) reported current e-cigarette use.91 Since 2014, e-cigarettes/vaping modules have been the most common nicotine delivery option for teens and young adults.91 These groups should be questioned about vaping as the potential for early nicotine abuse exists. Smoking is often not associated with the fruity flavors delivered in vapors.91,92 Roughly 85% of middle school and high school students will choose flavored options for vaping, with fruit flavors being the most popular option across all demographics.92 In addition to educating patients on the ocular risks associated with vaping, optometrists should also be prepared to provide resources to help individuals who are interested in cessation.
Risk Factor #3: Screen Time
Even the most robust tear film cannot fight the evaporative stress induced by excessive screen time. The actual amount of screen time associated with inducing dryness is shockingly low. Research revealed a correlation of as little as two hours of screen time daily with dry eye.93 A study of young adult computer users demonstrated statistically significant poorer symptomology correlated with increased screen use.94 The average adult in the United States spends around three to four hours daily on their smartphone, personal computer and other digital activities.95
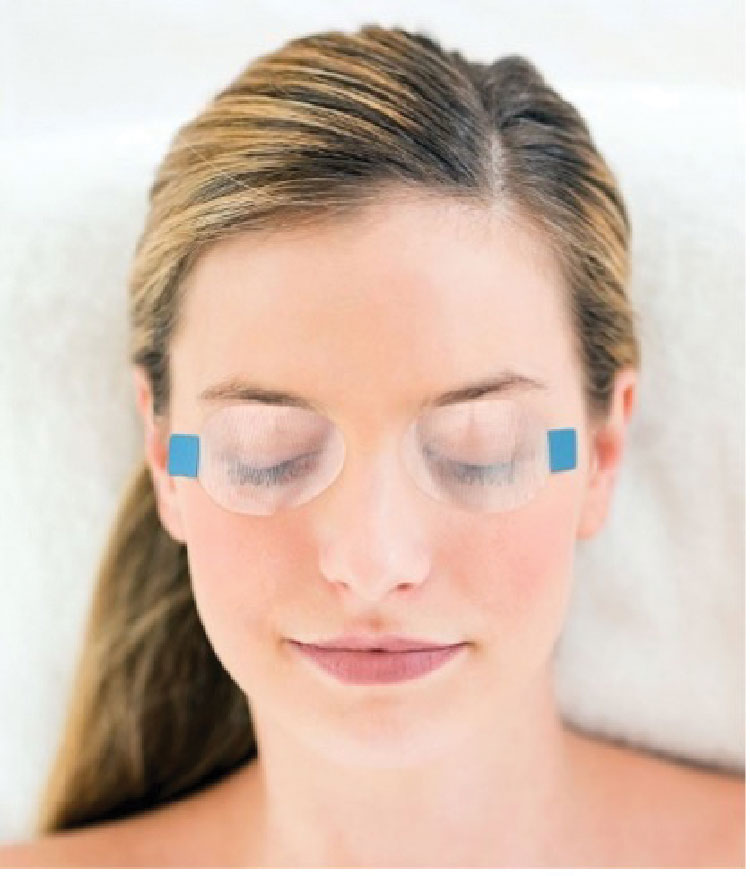 |
| Fig. 4. The Sleep Tite Sleep Rite shield is a newer option for managing lagophthalmos.112 Click image to enlarge. |
Evaporative stress occurs due to a lack of protective blinking during digital device use. Multiple studies have demonstrated that the regular resting blink rate of 17 to 23 blinks per minute is reduced to between 3.6 to 10 blinks per minute when on screens.96-98 Eyes simply are not being covered enough during screen time. Lack of blinking has also been positively associated with meibomian gland dysfunction and dry eye.99-103 The mechanism by which protective meibum is secreted onto the lid margin to be incorporated into the tears requires a complete blink. The muscles of Riolan (termination of the orbicularis oculi in the eyelid) contract with the complete blink, releasing meibum from the terminal ducts of the meibomian glands.104 The oil is then picked up by the upper eyelid and spread across the surface of the eye for incorporation in the tear film.104 Incomplete blinking equates to no meibum in the tear film, gland obstruction and inflammatory sequelae.
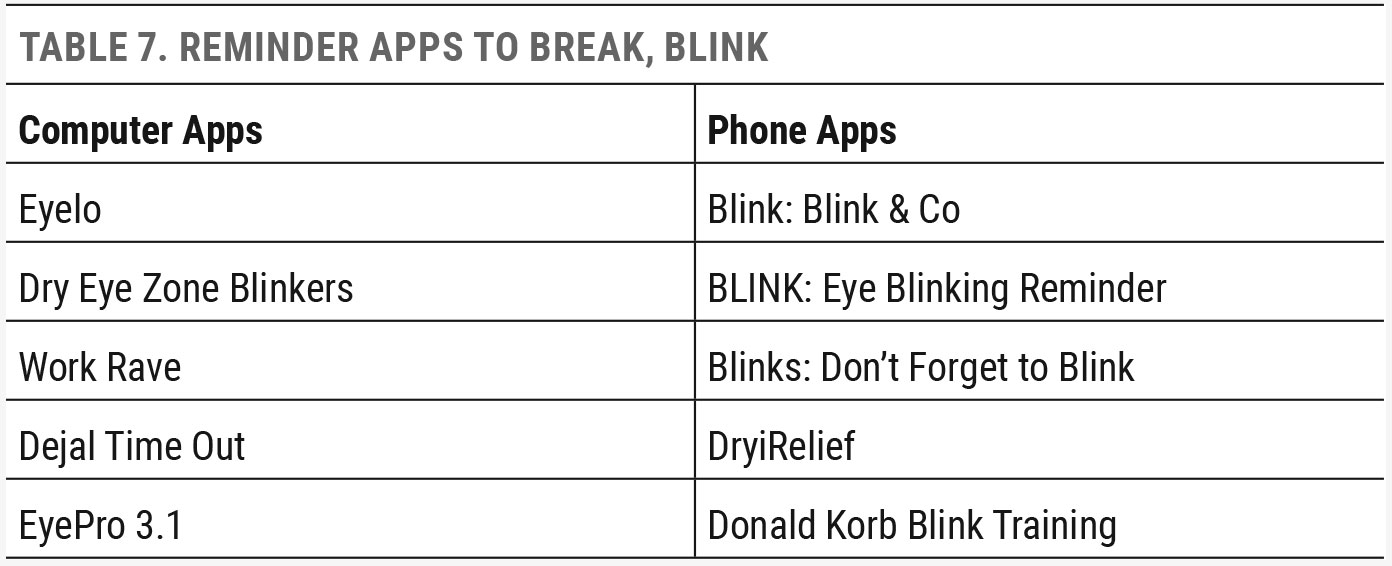
The combination of exposure coupled with inadequate volumes of meibum is a recipe for evaporative dry eye. Regular breaks and complete blinking can help to combat screen-associated dryness. There are a variety of free or inexpensive apps that can be installed onto both computers and smartphones that remind users to take healthy breaks and blink completely. Other workspace dry eye practices include humidifiers, air vent deflectors and moisture chamber/wind-blocking eyewear.
Even our younger patients are at risk, with children from eight to 12 years old spending four to six hours a day on screens, and teens facing up to nine hours of daily exposure.105 The American Academy of Child and Adolescent Psychology recommends all children take frequent breaks and stop all screen activity 30 to 60 minutes prior to going to sleep at night.104 Educating patients and their parents on the risks associated with excessive screen time is becoming increasingly important with the introduction of more and more digital devices.
Risk Factor #4: Sleep Issues
 |
| Click to enlarge. |
Screen-induced sleep perturbations, in addition to primary sleep disorders and medication-induced sleep problems, can also be major risk factors for dryness. Primary sleep disorders have been associated with a cycle of ocular surface damage and dry eye disease symptoms.106,107 Sleep disorders have been shown to lead to “decreased aqueous tear secretion, increased corneal epithelial cell defects, corneal sensitivity and apoptosis and induced squamous metaplasia of the corneal epithelium in animal models.107 There is normal diurnal variation in tear secretion, and this balance is interrupted by poor sleep.108 Obstructive sleep apnea (OSA) not only disrupts normal sleep but is also associated with decreased blood supply to the eye. A lack of normal blood supply leads to hypoxia and inflammation, with subsequent ocular surface damage.109 OSA is also associated with floppy eyelid syndrome, which could cause further nighttime irritation.110
The case history can illuminate whether patients have sleep risk factors for eye dryness. Any patient who is not obtaining help for sleep disorders should be encouraged to investigate undiagnosed sleep problems. A great place to refer patients to help start the conversation about poor sleep with their internal health provider is sleepeducation.org/patients.
 |
| Click to enlarge. |
A patient who wakes in the morning or throughout the night with symptoms of dryness should be examined for nocturnal lagophthalmos. While sleeping with partially open eyes can occur from top to bottom, anatomical variations and disease states like thyroid ophthalmopathy can also lead to gaps from front to back, like a dental overbite. Shining a penlight or transilluminator on the closed eyelid and examining the lid margin for escaping light can help to identify patients who may be at risk of ocular surface exposure at night.111 A new solution for nighttime exposure, in addition to nighttime lubricants and sleep shields, is the Sleep Tite Sleep Rite shield (Figure 4). These shields help to keep the eyelids closed and the ocular surface protected at night. Alternating from right to left every other night can help break the cycle of morning dryness.112
Takeaways
Excessive screen time, vaping/e-cigarette use, unhealthy eye cosmetics/enhancements and poor sleep can lead to daily chronic ocular irritation. These ocular surface dryness risk factors are primarily identifiable through a patient case history. Without attention to the lifestyle contributions to dry eye, the disease cannot be effectively treated. Digital resources are available to help guide eyecare practitioners and all patient types on healthier lifestyle options that promote and protect ocular surface health. It is important that optometrists are aware of modifiable risk factors of dry eye and how to best educate and support their patients.
 |
| Click to enlarge. |
 |
| Click to enlarge. |
Dr. Doll spent 15 years in academia and now practices at Sunset Eye Clinic in Beaverton, OR, where she is the director of ocular surface care services. She also serves on the American Academy of Optometry Anterior Segment Section leadership team and is a member of the Intrepid Eye Society and the Tear Film and Ocular Surface Society. She has a passion for lecturing, writing and conducting research on ocular surface dryness and eye beauty. Dr. Doll receives fees from Dompé, Oyster Point, Science-Based Health, Kala, Cynosure and Sun Pharma.
1. Craig JP, Nichols KK, Akpek EK, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017;15(3):276-83. 2. The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007;5(2):75-92. 3. TFOS Lifestyle Workshop. Tear Film and Ocular Surface Society. https://www.tearfilm.org/paginalong-tfos_lifestyle_workshop/7296_7295/eng/. 4. Eye cosmetic sales in the United States in 2019, by segment. Stastia.com. https://www.statista.com/statistics/538035/us-eye-cosmetic-sales-by-segment/. 5. Pikoos TD, Buzwell S, Sharp G, et al. The Zoom Effect: Exploring the Impact of Video Calling on Appearance Dissatisfaction and Interest in Aesthetic Treatment During the COVID-19 Pandemic. Aesthet Surg J. 2021;41(12):NP2066-75. 6. Chen J, Chow A, Fadavi D, et al. The Zoom Boom: How Video Calling Impacts Attitudes Towards Aesthetic Surgery in the COVID-19 Era. Aesthet Surg J. 2021;41(12):NP2086-93. 7. Pfund GN, Hill PL, Harriger J. Video chatting and appearance satisfaction during COVID-19: Appearance comparisons and self-objectification as moderators. Int J Eat Disord. 2020;53(12):2038-43. 8. Aslan Kayıran M, Kara Polat A, Alyamaç G, et al. Has the COVID-19 pandemic changed attitudes and behaviors concerning cosmetic care and procedures among patients presenting to the dermatology outpatient clinic? A multicenter study with 1437 participants. J Cosmet Dermatol. 2021;20(10):3121-7. 9. U.S. Food & Drug Administration. Prohibited & Restricted Ingredients in Cosmetics. https://www.fda.gov/Cosmetics/GuidanceRegulation/LawsRegulations/ucm127406.htm#differentingredients. 10. U.S. Food & Drug Administration. “Hypoallergenic” Cosmetics. https://www.fda.gov/Cosmetics/Labeling/Claims/ucm2005203.htm. 11. Adams RM, Maibach HI. A five-year study of cosmetic reactions. Journal of the American Academy of Dermatology. J Am Acad Dermatol. 1985;13(6):1062-9. 12. Meynadier JM, Meynadier J, Mark Y. True cosmetic-induced dermatitis. In: Baran R, Maibach HI, 1st ed. Textbook of Cosmetic Dermatology. London, UK, Martin Dunitz, 1994:551-6. 13. Takagi Y, Kaneda K, Miyaki M, et al. The long-term use of soap does not affect the pH-maintenance mechanism of human skin. Skin Res Technol. 2014;21:144-8. 14. Lambers H, Piessens S, Bloem A, et al. Natural skin surface pH is on average below 5, which is beneficial for its resident flora. Int J Cosmet Sci. 2006;28(5):359-70. 15. Schmid-Wendtner MH, Korting HC. The pH of the skin surface and its impact on the barrier function. Skin Pharmacol Physiol. 2006;19(6):296-302. 16. Pflanzer, LR. What those ‘Dermatologist Recommended’ and ‘Clinically Proven’ labels on your lotions and soap actually mean. http://www.businessinsider.com/what-does-clinically-proven-mean-2015-10. 17. Environmental Working Group SkinDeep Database. https://www.ewg.org/skindeep/. 18. Clearya Chrome Extension and Mobile App. clearya.com. 19. Cosmetic Calculator. Cosmetic and Perfume Batch Code Analyzer. https://m.checkcosmetic.net/. 20. Think Dirty App. https://thinkdirtyapp.com/. 21. Ingredio Beta Ingredients Screener App. 22. Vadillo, Raul. Ingred Cosmetic and Food Analysis App. 23. Draelos ZD. Special considerations in eye cosmetics. Clin Dermatol. 2001;19:424-30. 24. Orecchinoi AM. Eye make-up. In: Baran R, Maibach HI, eds. Cosmetic. Dermatology. London, UK, Martin Dunitz, 1994. pp. 143-9. 25. Hagvall L, Rudbäck J, Bråred Christensson J, et al. Patch testing with purified and oxidized citronellol. Contact Dermatitis. 2020;83(5):372-9. 26. Environmental Working Group. CITRONELLOL. Environmental Working Group SkinDeep Database. https://www.ewg.org/skindeep/ingredients/701389-CITRONELLOL/. 27. National Center for Biotechnology Information. PubChem Compound Summary for CID 8842, Citronellol. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/3_7-dimethyloct-6-en-1-ol. 28. Environmental Working Group. GERANIOL. Environmental Working Group SkinDeep Database. https://www.ewg.org/skindeep/ingredients/702568-geraniol/. 29. National Center for Biotechnology Information. PubChem Compound Summary for CID 637566, Geraniol. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Geraniol. 30. Environmental Working Group. Linalool. https://www.ewg.org/skindeep/ingredients/703568-LINALOOL/. 31. National Center for Biotechnology Information. PubChem Compound Summary for CID 6549, Linalool. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Linalool. 32. Yazar K, Johnsson S, Lind ML, et al. Preservatives and fragrances in selected consumer-available cosmetics and detergents. Cont Dermat. 2011;64(5):265–72. 33. Environmental Working Group. METHYLPARABEN. https://www.ewg.org/skindeep/ingredients/703937-methylparaben/. 34. National Center for Biotechnology Information. PubChem Compound Summary for CID 7456, Methylparaben. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Methylparaben. 35. Environmental Working Group. PROPYLPARABEN https://www.ewg.org/skindeep/ingredients/705335-propylparaben/. 36. National Center for Biotechnology Information. PubChem Compound Summary for CID 8434, Ethylparaben. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Ethylparaben. 37. Environmental Working Group. ETHYLPARABEN. https://www.ewg.org/skindeep/ingredients/702355-ethylparaben/. 38. National Center for Biotechnology Information. PubChem Compound Summary for CID 7175, Propylparaben. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Propylparaben. 39. Environmental Working Group. BUTYLPARABEN. https://www.ewg.org/skindeep/ingredients/700868-butylparaben/. 40. National Center for Biotechnology Information. PubChem Compound Summary for CID 7184, Butylparaben. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Butylparaben. 41. Environmental Working Group. ISOBUTYLPARABEN. https://www.ewg.org/skindeep/ingredients/703160-isobutylparaben/. 42. National Center for Biotechnology Information. PubChem Compound Summary for CID 20240, Isobutyl 4-hydroxybenzoate. 2022. https://pubchem.ncbi.nlm.nih.gov/compound/Isobutyl-4-hydroxybenzoate. 43. DeGroot AC, Flyvholm MA, Lensen G, et al. Formaldehyde-releasers: relationship to formaldehyde contact allergy. Contact allergy to formaldehyde and inventory of formaldehyde-releasers. Contact Dermatitis. 2009;61(2):63-85. 44. Harley KG, Berger KP, Kogut K, et al. Association of phthalates, parabens and phenols found in personal care products with pubertal timing in girls and boys. Hum Reprod. 2019;34(1):109-17. 45. Berger KP, Kogut KR, Bradman A, et al. Personal care product use as a predictor of urinary concentrations of certain phthalates, parabens, and phenols in the HERMOSA study. J Expo Sci Environ Epidemiol. 2019;29(1):21-32. 46. Aerts O, Verhulst L, Goossens A. Ethylhexylglycerin: a low-risk, but highly relevant, sensitizer in ‘hypo-allergenic’ cosmetics. Contact Dermatitis. 2016;74(5):281-8. 47. Langsrud S, Steinhauer K, Lüthje S, et al. Ethylhexylglycerin Impairs Membrane Integrity and Enhances the Lethal Effect of Phenoxyethanol. PLoS One. 2016;11(10):e0165228. 48. Wang Q, Cui S, Zhou L, et al. Effect of cosmetic chemical preservatives on resident flora isolated from healthy facial skin. J Cosmet Dermatol. 2019;18(2):652-8. 49. Norek, D. Four common formaldehyde releasers to avoid in your cosmetics and skin care. 2013. https://www.naturalnews.com/041323_formaldehyde_skin_care_cosmetics.html. 50. Environmental Working Group. Iron Oxides. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/706410-iron-oxides/. 51. Environmental Working Group. Titanium Dioxide. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/706561-titanium-dioxide/. 52. Environmental Working Group. Copper Gluconate. https://www.ewg.org/skindeep/ingredients/701642-copper-gluconate/. 53. Environmental Working Group. Aluminum Hydroxide. https://www.ewg.org/skindeep/ingredients/700321-aluminum-hydroxide/. 54. Environmental Working Group. Ultramarines. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/706769-ultramarines/. 55. Environmental Working Group. Manganese Violet. https://www.ewg.org/skindeep/ingredients/703741-manganese-violet/. 56. Environmental Working Group. Carmine. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/701120-carmine/. 57. Environmental Working Group. Chromium Oxide. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/757066-chromium-oxide/. 58. Environmental Working Group. Ferric Ferrocyanide. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/702454-ferric-ferrocyanide/. 59. Environmental Working Group. Bismuth Oxychloride. SkinDeep Database. https://www.ewg.org/skindeep/ingredients/700778-bismuth-oxychloride/. 60. Kim HW, Choi YJ, Lee KW, et al. Periorbital changes associated with prostaglandin analogs in Korean patients. BMC Ophthalmology. 2017; doi:10.1186/s12886-017-0521-4. 61. Lee TH, Sung MS, Heo H, et al. Association between meibomian gland dysfunction and compliance of topical prostaglandin analogs in patients with normal tension glaucoma. PLoS One. 2018;13(1):e0191398. 62. T.Doll, et al. Over-the-Counter Eyelash Growth Serum Use: Self-Reported Pervasiveness and User Satisfaction. Association for Research in Vision and Ophthalmology (ARVO) meeting. 2020. Poster #3365497. 63. Pharmaceutical Ingredients in one out of three eyelash serums. Swedish Medical Products Agency Report. 2013. https://www.dr-jetskeultee.nl/jetskeultee/download/common/artikel-wimpers-ingredients.pdf. 64. Pyo HK, Yoo HG, Won CH, et al. The effect of tripeptide-copper complex on human hair growth in vitro. Arch Pharm Res. 2007;30(7):834-9. 65. Iwabuchi T, Takeda S, Yamanishi H, et al. The topical penta-peptide Gly-Pro-Ile-Gly-Ser increases the proportion of thick hair in Japanese men with androgenetic alopecia. J Cosmet Dermatol. 2016;15(2):176-84. 66. Pyo HK, Yoo HG, Won CH, et al. The effect of tripeptide-copper complex on human hair growth in vitro. Arch Pharm Res. 2007;30(7):834-9. 67. Iwabuchi T, Takeda S, Yamanishi H, et al. The topical penta-peptide Gly-Pro-Ile-Gly-Ser increases the proportion of thick hair in Japanese men with androgenetic alopecia. J Cosmet Dermatol. 2016;15(2):176-84. 68. Amador GJ, Mao W, DeMercurio P, et al. Eyelashes divert airflow to protect the eye. J R Soc Interface. 2015;12(105):20141294. 69. Pack LD, Whickham MG, Enole RA, et al. Microbial contamination associated with mascara use. Optometry 2008;79:587–93. 70. Adamowicz MS, Labonte RD, Schienman JE. The Potential of Cosmetic Applicators as a Source of DNA for Forensic Analysis. J Forensic Sci. 2015;60(4):1001-11. 71. Naz S, Iqtedar M, Ain Q, et al. Incidence of Human Skin Pathogens from Cosmetic Tools used in Beauty Saloons from Different Areas of Lahore, Pakistan. Journal of Scientific Research. 2012;4(2):523-7. 72. Corazza M, Carla E, Rossi MR, et al. Face and body sponges: beauty aids or potential microbiological reservoir? Eur J Dermatol. 2003;13(6):571-3. 73. Bashir A, Lambert P. Microbiological study of used cosmetic products: highlighting possible impact on consumer health. J Appl Microbiol. 2020;128(2):598-605. 74. Ortiz V. Effectiveness of commercially-available cosmetic cleaners on cosmetics and cosmetic brushes, Master Thesis, The Graduate College, The University of Nevada, Las Vegas, April 14, 2016. https://www.semanticscholar.org/paper/Effectiveness-of-Commercially-Available-Cosmetic-on-Ortiz/d4c0b451ce31cadd584ae5a3bfb306d53a16a41f. 75. Christian Giroud, Mariangela de Cesare, Aurélie Berthet, Vincent Varlet, Nicolas Concha-Lozano, and Bernard Favrat, CC BY 4.0, via Wikimedia Commons. https://upload.wikimedia.org/wikipedia/commons/f/f2/Ijerph_ecig_construction.jpg. 76. Miskinis C. How digital twins will impact E-cig manufacturing and production. 2018. https://www.challenge.org/insights/digital-twin-vaporizer/. 77. Stanford Medicine. E-Cigarette and Vape Pen Module. https://med.stanford.edu/tobaccopreventiontoolkit/curriculum-decision-maker/by-module/E-Cigs.html. 78. Goniewicz ML, Knysak J, Gawron M, et al. Levels of selected carcinogens and toxicants in vapour from electronic cigarettes. Tob Control. 2014 Mar;23(2):133-9. 79. Rowell TR, Tarran R. Will chronic e-cigarette use cause lung disease? Am J Physiol Lung Cell Mol Physiol. 2015 Dec 15;309(12):L1398-409. 80. Thirión-Romero I, Pérez-Padilla R, Zabert G, et al. RESPIRATORY IMPACT OF ELECTRONIC CIGARETTES AND “LOW-RISK” TOBACCO. Rev Invest Clin. 2019;71(1):17-27. 81. Martheswaran T, Shmunes MH, Ronquillo YC, et al. The impact of vaping on ocular health: a literature review. Int Ophthalmol. 2021;41(8):2925-32. 82. Moroz, K. Dry Eyes and Vaping: Are Your Patients at Risk? https://ophthalmology360.com/print-exclusives/dry-eyes-and-vaping-are-your-patients-risk/. 83. Mastrota, KM. How vaping affects the ocular surface. 2017. https://www.optometrytimes.com/view/modern-medicine-feature-how-vaping-affects-ocular-surface. 84. Md Isa NA, Doraj P, Koh PY. The Impact Of E-Cigarette Smoking And Vaping Voltage On Tear Film. International Journal Of Allied Health Sciences. 2021;5(3):2272. 85. Miglio F, Naroo S, Zeri F, et al. The effect of active smoking, passive smoking, and e-cigarettes on the tear film: An updated comprehensive review. Exp Eye Res. 2021;210:108691. 86. Munsamy A, Bhanprakash B, Sirkhot A, et al. A pre-test post-test assessment of non-invasive keratograph break up time and corneal epithelial thickness after vaping. Afr Health Sci. 2019;19(4):2926-33. 87. Makrynioti D, Zagoriti Z, Koutsojannis C, et al. Ocular conditions and dry eye due to traditional and new forms of smoking: A review. Cont Lens Anterior Eye. 2020;43(3):277-84. 88. Paley GL, Echalier E, Eck TW, et al. Corneoscleral Laceration and Ocular Burns Caused by Electronic Cigarette Explosions. Cornea. 2016;35(7):1015-18. 89. Dekhou A, Oska N, Partiali B, et al. E-Cigarette Burns and Explosions: What are the Patterns of Oromaxillofacial Injury? J Oral Maxillofac Surg. 2021;79(8):1723-30. 90. Ocran C, Chaum E, Sobel RK. Vaping May Be Hazardous to Your Eye. Ophthalmology. 2020;127(12):1756. 91. Park-Lee E, Ren C, Sawdey MD, et al. Notes from the Field: E-Cigarette Use Among Middle and High School Students — National Youth Tobacco Survey, United States, 2021. MMWR Morb Mortal Wkly Rep 2021;70:1387-9. 92. Park L, Klein D. Teens and Vaping: What’s the Latest Trend. Proceedings of the 18th International RAIS Conference, August 17-18, 2020, Research Association for Interdisciplinary Studies. 93. Andrews J. The impact of digital devices on meibomian gland structure and function. Presented at: American Academy of Optometry meeting; Orlando, Fla.; Oct. 23-27, 2019. 94. Muntz A, Turnbull PR, Kim AD, et al. Extended screen time and dry eye in youth. Cont Lens Anterior Eye. 2021:101541. 95. Zalani R. Screen Time Statistics 2021: Your Smartphone Is Hurting You. 2021. https://elitecontentmarketer.com/screen-time-statistics/. 96. Bentivoglio AR, Bressman SB, Cassetta E, et al. Analysis of blink rate patterns in normal subjects. Mov Disord. 1997;12:1028-34. 97. Tsubota K, Nakamori K. Dry eyes and video display terminals. N Engl J Med. 1993;328(8):584. 98. Schlote T, Kadner G, Freudenthaler N. Marked reduction and distinct patterns of eye blinking in patients with moderately dry eyes during video display terminal use. Graefes Arch Clin Exp Ophthalmol. 2004;242(4):306-12. 99. Hirota M, Uozato H, Kawamorita T, et al. Effect of incomplete blinking on tear film stability. Optom Vis Sci. 2013;90(7):650-7. 100. Kawashima M, Tsubota K. Tear lipid layer deficiency associated with incomplete blinking: a case report. BMC Ophthalmol. 2013;13:34. 101. Kojima T, Ibrahim OM, Wakamatsu T, Tsuyama A, Ogawa J, Matsumoto Y, Dogru M, Tsubota K. The impact of contact lens wear and visual display terminal work on ocular surface and tear functions in office workers. Am J Ophthalmol. 2011;152(6):933-940.e2. 102. Portello JK, Rosenfield M, Chu CA. Blink rate, incomplete blinks and computer vision syndrome. Optom Vis Sci. 2013;90(5):482-7. 103. McMonnies CW. Incomplete blinking: exposure keratopathy, lid wiper epitheliopathy, dry eye, refractive surgery, and dry contact lenses. Cont Lens Anterior Eye. 2007;30(1):37-51. 104. Braun RJ, King-Smith PE, Begley CG, et al. Dynamics and function of the tear film in relation to the blink cycle. Prog Retin Eye Res. 2015;45:132-64. 105. American Academy of Child and Adolescent Psychology. Screen Time and Children. 2020. https://www.aacap.org/AACAP/Families_and_Youth/Facts_for_Families/FFF-Guide/Children-And-Watching-TV-054.aspx. 106. Magno MS, Utheim TP, Snieder H, et al. The relationship between dry eye and sleep quality. Ocul Surf. 2021;20:13-19. 107. Li S, Ning K, Zhou J, et al. Sleep deprivation disrupts the lacrimal system and induces dry eye disease. Exp Mol Med. 2018;50(3):e451. 108. Walker PM, Lane KJ, Ousler GW 3rd, et al. Diurnal variation of visual function and the signs and symptoms of dry eye. Cornea. 2010;29(6):607-12. 109. Zhang LL, Song L, Fan YF, et al. [Changes of ophthalmic blood flow in obstructive sleep apnea-hypopnea syndrome]. Zhonghua Yan Ke Za Zhi. 2012;48(7):631-6. 110. Cristescu Teodor R, Mihaltan FD. Eyelid laxity and sleep apnea syndrome: a review. Rom J Ophthalmol. 2019;63(1):2-9. 111. Blackie CA, Korb DR. A novel lid seal evaluation: the Korb-Blackie light test. Eye Contact Lens. 2015;41(2):98-100. 112. Sleep Tite Sleep Rite Website. https://www.eyesleeptite.com/. |
